

Ingrown Toenails
We have all made the painful mistake of trimming our nails too short at some point in our lives. Sometimes, this can really affect our foot health by causing ingrown toenails.
This happens when the nail grows downward into the skin instead of straight out, usually causing an infection. Ingrown toenails are most common on the sides of the big toe. It can also be caused by shoe pressure, injury, fungal infections, poor foot structure, etc.
Warm water soaks several times a day, properly fitted shoes and socks, and trimming nails in a straight line (rather than rounded) are ways to treat and prevent painful ingrown toenails. If there is an infection, antibiotics may be prescribed.
FAQ
What is an ingrown toenail?
An ingrown toenail occurs when the edge of your toenail grows into your soft flesh. Any of your toes can develop an ingrown nail but it most commonly affects the big toe. In many cases, an ingrown toenail can cause a break in the skin leading to an infection. If left untreated, the infection caused by an ingrown toenail can reach the underlying bone.
Ingrown toenails are especially dangerous for people with diabetes or other conditions that affect the nerves and blood flow in the feet. If you suffer from diabetes, a simple ingrown toenail can lead to an open sore or gangrene. Although the symptoms of an ingrown toenail can be quite painful, the condition is highly treatable.
What are the symptoms of an ingrown toenail?
Symptoms of an ingrown toenail include:
- Swelling or redness around your nail
- Tenderness
- Warmth
The pain caused by an ingrown toenail may worsen as the nail continues to dig into your skin. If you notice symptoms, book an appointment at Foot & Ankle Institute of Utah to find out the best treatment for your condition. You should especially seek medical treatment if you have diabetes or if you notice pus draining from the affected toe.
How are ingrown toenails treated?
Treatment depends on the severity of your condition. Many people experience relief with at-home care. If your condition is mild, our doctors may recommend soaking the affected foot or using over-the-counter pain relievers. They may also perform a simple splinting procedure to lift the affected nail and help it grow normally.
If your condition is severe or doesn’t go away with conservative treatment, our providers may have to remove parts of your nail and the underlying tissue. Our providers have extensive experience successfully treating ingrown toenails with a very low recurrence rate.
How can I prevent ingrown toenails?
After treatment, there are steps you can take to reduce your risk of future ingrown toenails. For starters, you should always wear shoes that fit properly. Ill-fitting footwear can put too much pressure on your toes, causing your toenails to grow abnormally. You should also be sure to follow proper nail care, trimming your nails straight across and keeping them at a moderate length. If you have diabetes, make sure to check your feet regularly for ingrown toenails and other foot problems.

Bunions
A bunion is a bony bump that forms on the joint at the base of your big toe. They can develop from an inherited structural defect, excess stress on your foot, or can result from an existing medical condition.
For the most part, bunions require no medical treatment. However, if you are experiencing one or more of the following, a podiatrist can help alleviate your symptoms.
FAQ
What is a bunion?
A bunion is a bony growth that develops on the inside of your foot near the base of your big toe. Unlike a corn or callus that involves the skin of your foot, bunions affect the structure of the bones in your feet.
A bunion occurs when the bones in the front of your foot begin to shift out of place. This causes the tip of your big toe to gradually point inward, exposing the joint at the base of your big toe.
Bunions can cause a number of uncomfortable symptoms, including swelling, redness, and ongoing foot pain. A tell-tale sign of a bunion is a bulging bump on the outside of your big toe. Bunions that develop on your smaller toes are called bunionettes.
What causes bunions?
Bunions can be caused by a number of different factors. For many people, the natural structure of their feet leaves them more prone to bunions. Foot stress and foot injuries can also cause you to develop bunions. Wearing high heels or tight-fitting shoes is another factor that can increase your risk of developing bunions. If left untreated, bunions can lead to further problems with the joints in your foot as well as other foot deformities like hammertoe.
Do I have bunions?
A bunion is a progressive condition that happens gradually over time. As the bunion grows, your condition becomes more painful and difficult to cope with. If you notice abnormal bending of your big toe or it’s becoming increasingly painful to wear your normal footwear, you may be suffering from a bunion.
At Foot & Ankle Institute of Utah, our providers performs thorough evaluations to properly diagnose painful bunions. During your appointment, a provider performs a physical exam as well as the necessary imaging tests to evaluate your condition. Once you’ve been diagnosed, a provider works with you to determine the best way to treat your bunion.
How are bunions treated?
There are a number of safe and effective ways to treat bunions. In many cases, bunion pain can be relieved with simple steps like changing your footwear or applying ice to sore or swollen feet. We offer custom orthotics to help relieve the pressure on your bunion and improve the alignment of your feet.

Calluses
Calluses, on the other hand, don’t usually cause pain. They usually develop on the soles of your feet, especially under the heels or balls, on your palms, or on your knees. Calluses vary in size and shape and are often larger than corns.

Hammertoes
Hammertoe is a deformity where one or both joints of the second, third, fourth or fifth toes begin to bend outside of their normal alignment. Pressure can begin to weigh heavy on the toes as you wear shoes which is where pain and other symptoms develop.
Hammertoes typically begin with small symptoms and deformities and continue to worsen with time. In its beginning stages, hammertoes are often impressionable which means they can be controlled using minimal treatment. It is important to know the signs of hammertoes to get them evaluated early. If left untreated, hammertoes can become more firm and difficult to manipulate, requiring surgery.
FAQ
What are hammertoes?
Hammertoes are a deformity that affects the joints in your toe. The condition can affect any of your four smaller toes and causes the affected toes to bend abnormally at the middle joint.
Hammertoes can cause a number of concerning symptoms, including inflammation, redness, and burning pain. It can also cause calluses and corns to develop on your toes and the ball of your foot.
Left untreated, hammertoes can result in the affected toes becoming rigid and stiff, causing them to become permanently bent.
What causes hammertoes?
A number of things can contribute to the development of hammertoes. Wearing high-heeled or tight-fitting shoes can crowd your toes and increase your risk of developing hammertoes. Breaking a toe or severely stubbing it can also cause hammertoes.
In most cases, hammertoes are caused by an imbalance of the tendons and muscles in your toe. This imbalance causes the toe to become unstable and eventually to contract.
How are hammertoes treated?
Your treatment begins with an accurate diagnosis. In most cases, hammertoes are diagnosed during a simple physical exam.
If you suffer from hammertoes, it’s important to seek medical treatment as the condition won’t clear up on its own. We specialize in conservative treatment of hammertoe. Your treatment can include:
- Changing your footwear
- Using custom orthotics (shoe inserts)
- Trimming corns and calluses
- Taking anti-inflammatory medicine
- Splinting your foot
Wearing tight shoes or high heels can aggravate your hammertoes and intensify your pain. Choosing the right footwear can relieve pressure on your toes and eliminate your painful symptoms.

Diabetic Foot Care
Daily preventative care can help you decrease your risk of developing these other serious conditions like ulcers and infections. Inspecting your feet at the end of the day to look for any abnormalities, maintaining proper hygiene, keeping your feet warm in cold weather, encouraging blood flow in the feet, and maintaining an overall healthy lifestyle can discourage other conditions from developing.

Warts
Plantar warts are caused by the HPV virus and cause tiny cuts and breaks on the bottom of your feet.
While most plantar warts are not a major health concern, it is advised you see a doctor to have the warts examined and removed. Some symptoms include small, rough lesions on the base of the foot, calluses in one spot, and tenderness when walking or standing for long periods of time.
FAQ
How do you get warts?
Plantar warts are most likely passed from person to person indirectly. The time from the first contact to the time when the lesion can be visualized may be several months. The risk of “catching” hand or foot warts is small. Other warts may be more contagious.
How are warts treated?
Cryotherapy (freezing) is often used in children, however, this method does seem to work well with plantar warts due to the heavy skin on the sole of the foot. Electrosurgery and or laser surgery can be used for treatment on a single visit to the operating room. This method often requires non-weight bearing to lessen the scarring affect from the surgery. Scars from wart removal can be painful and will be permanent. The surgical methods are usually reserved for a very large area, or for those lesions that do not respond to office based treatments. The most commonly used method for treating warts is through topical acid agents that cause blisters to form around the lesion, or chemicals that help the immune system to attack the lesions. The topical blistering agent (cantharidin) causes a blister to form under the wart. The blister can then be clipped away, removing the dead part of the wart in the blister roof. This process can take up to 3 or more visits, depending on how resistant the lesion is to treatment. Immunotherapy treatments attempt to build up the body’s own reaction/rejection system. Several methods of immunotherapy are being tried. With one method, the patient is made allergic to a certain chemical which is painted on the wart(s). A mild allergic reaction occurs around the treated wart(s), and may result in the disappearance of the wart(s).
What about recurrent warts?
TUE Sometimes it seems as if new warts appear as fast as old ones go away. This may happen because old warts have shed viruses into the stranding surrounding skin before they were treated. In reality, new “baby” warts are growing up around the original “mother” warts. The best way to limit this is to treat new warts as quickly as they develop so they have little time to shed viruses into the nearby skin. If you have questions regarding recurrence, a check-up by your healthcare provider would be helpful. Immunocompromised patients including diabetics or those on chemotherapy or drugs for arthritis may be more prone to develop warts and to have a reoccurrence of the lesions.

Heel Spurs/Plantar Fasciitis
Heel spurs occur in at least 50% of people who have plantar fasciitis. Past treatments for heel spurs, a bony growth that begins on the front of your heel bone and points toward the arch of your foot, included surgery to remove the growth. Nowadays, surgery is rarely a treatment option and more plans for physical therapy, ice, and pain medications are used to treat heel spurs.
FAQ
What is plantar fasciitis?
Most cases of heel pain can be linked to plantar fasciitis. Plantar fasciitis occurs when the band of tissue called the plantar fascia is inflamed. The plantar fascia runs along the bottom of your foot and connects your heel to the front of your foot.
The most common sign of plantar fasciitis is a stabbing pain that increases after standing or resting for long periods of time. Many people experience the stabbing pain of plantar fasciitis first thing in the morning.
What causes plantar fasciitis?
The tissues along the bottom of your foot absorb a lot of stress as you walk. If too much stress is placed on this tissue, stretching and tearing can occur, eventually leading to plantar fasciitis. There are a number of factors that contribute to plantar fasciitis, including:
- Age
- Obesity
- Certain exercises
Plantar fasciitis most commonly affects people between the ages of 40 and 60. Plantar fasciitis is also common among runners and people who spend much of their workday walking or standing. Having flat feet or high arches can increase your risk of developing plantar fasciitis. Left untreated, plantar fasciitis can alter the way you walk, leading to problems with your hips, knees, and back.
How is plantar fasciitis diagnosed?
To diagnose your condition, We begin with a discussion of your symptoms and a physical exam. During the exam, we feel for the area of your pain. Identifying the location of your pain helps determine the cause. In some cases, imaging tests may be necessary to accurately diagnose your condition.
How is plantar fasciitis treated?
Most of the time, plantar fasciitis is successfully treated with conservative care. Conservative treatment may include:
- Over-the-counter pain relievers
- Rest
- Ice
- Night splints
- Orthotics
- Physical therapy
- Injections

Flat Feet
Do you have flat feet? Have you ever been told you or your kids would grow out of it? There are many misconceptions about flat feet, and it takes a thorough evaluation to ensure proper treatment. You may hear some terms that are synonymous with flat feet such as pes planus, posterior tibial tendon dysfunction (PTTD), talar declination, decreased calcaneal pitch, foot or ankle valgus. Not all flat feet are created equal and many are very complex biomechanical problems. There are 4 main stages of pes planus including mild deformity, moderate but flexible deformity, severe or ridged deformity, and those involving the ankle joint. There are many conservative and surgical treatment options. Orthotics, change in shoe gear and physical therapy. In some cases these conservative measures can completely resolve your symptoms. There are many advances in the foot and ankle specialty to correct flat feet surgically. There has never been a time when foot and ankle surgeons have been more empowered through clinical studies, evolution of techniques, improvement in hardware and biologics to help correct your flat feet. We have extensive experience correcting flat feet deformities of all kinds and at all life stages. Whether by conservative or surgical methods, his goal is always to help improve your quality of life.

Achilles Tendonitis
Achilles tendinitis is caused by overuse of the band of tissues that connects the lower region of your calf muscle to your heel bone, also known as your Achilles tendon. Those at a higher risk for Achilles tendinitis are runners engaging in intense training or middle-aged people who participate in sports on occasion.
FAQ
What is the Achilles Tendon?
The Achilles tendon is the largest tendon in the body. It is a powerful tendon extending from the calf muscles to the back of the heel. It provides immense power in push off while walking and running. In recent years we have discovered that through proper eccentric exercises the Achilles tendon can be strengthened in both tensile strength and in tissue mass. Up until this physiologic discovery was made, we often thought that the “Achilles heel” (Achilles tendon) was one of the limiting factors to athletic performance. Rupture of the Achilles tendon has sidelined many athletes over the years and has often been career ending, as these athletes are unable to regain full strength.
Acute inflammation of a tendon is called tendonitis. Tendonitis occurs from overuse in sports, excessively tight gastrocnemius and soleus muscles (calf muscles), poorly fitting shoes and improper biomechanical function as well as mechanical deformities. Swelling and abnormal popping of the tendon (crepitus) with or without nodular scar tissue formation is common in this condition. Left in a chronically inflamed state the tendon can develop tendinosis and begin to weaken and degenerate eventually leading to rupture. Carefully designed physician and therapist guided strengthening exercises along with improved mechanics can assist in providing an excellent outcome to this nagging disease.
As noted above, tendinosis develops from chronic tendinitis which has not been cared for properly. A condition called liquefaction necrosis can develop within the Achilles tendon leading to significant weakness and eventually to Achilles rupture when treated improperly. The classification of tendinosis is usually made after 3 months of chronic tendinitis and is clinically diagnosed by physical exam and through the use of MRI studies to determine the extent of damage.

Neuromas
A neuroma can occur in many areas of the body when nerve tissue thickens. Morton’s neuroma is the most typical neuroma that occurs in the foot and it occurs between the third and fourth toes. Also known as an intermetatarsal neuroma, the name describes its location in the ball of the foot.
Compression and irritation typically cause the nerve tissue to thicken. This pressure creates inflammation of the nerve, ultimately causing damage to the nerves in the foot.
FAQ
What is a neuroma?
A neuroma refers to abnormal growth of nerve tissue. The most common type of neuroma is Morton’s neuroma, a painful condition that occurs between your third and fourth toes. Morton’s neuroma causes the nerves in your foot to become enlarged. If left untreated, Morton’s neuroma can lead to permanent nerve damage. Although Morton’s neuroma is the most common, neuromas can affect other areas of your foot as well.
What causes neuromas?
Neuromas develop in response to compression or irritation of your nerves. One of the leading causes of Morton’s neuroma is wearing tight-fitting or high-heeled shoes. Tight-fitting shoes place unnecessary pressure on your toes and the ball of your foot.
Repetitive stress from activities like running and jogging is another leading cause of Morton’s neuroma. People with certain foot deformities like bunions, flat feet, or hammertoes are also at a higher risk of developing neuromas.
What are the symptoms of a neuroma?
Neuromas result in sharp, burning pain, as well as tingling numbness. Many people with Morton’s neuroma describe the condition as the feeling of standing on a pebble. The pain of Morton’s neuroma is typically felt in the ball of the foot and may radiate into your toes.
How are neuromas diagnosed?
To diagnose your condition, our providers begin with a physical examination, feeling for any tenderness or abnormalities in your foot. They may conduct imaging tests, such as an X-ray or ultrasound, to accurately identify your neuroma. After your diagnosis, you and the physician work together to determine the best treatment for you.
How are neuromas treated?
In most cases, treatment for your neuroma begins with conservative measures. We may recommend changing your footwear or taking over-the-counter anti-inflammatory medications to relieve your pain. We also offers injections and custom orthotics designed to relieve the pressure on the nerve.

Ankle Sprains
A sprained ankle occurs when you twist your ankle in an abnormal way causing the ligaments holding your ankle bones together to stretch or tear. Most sprained ankles involve injuries to the ligaments on the outer side of the ankle. Treatment for a sprained ankle depends on the severity of the injury. Although you may just need proper rest and pain medications to heal, it is important to have the sprain looked at by a professional to determine the severity and proper treatment.

Toenail Fungus
Fungal infections in the toe or fingernails can appear as thickened, discolored, or disfigured. While it may seem like the condition is just an aesthetic concern, fungal infections can lead to worsened symptoms and pain. Diabetes, a weakened immune system, and the normal aging process are all causes associated with fungal infections. It is more likely for senior citizens and adults to develop a fungal infection as opposed to children.
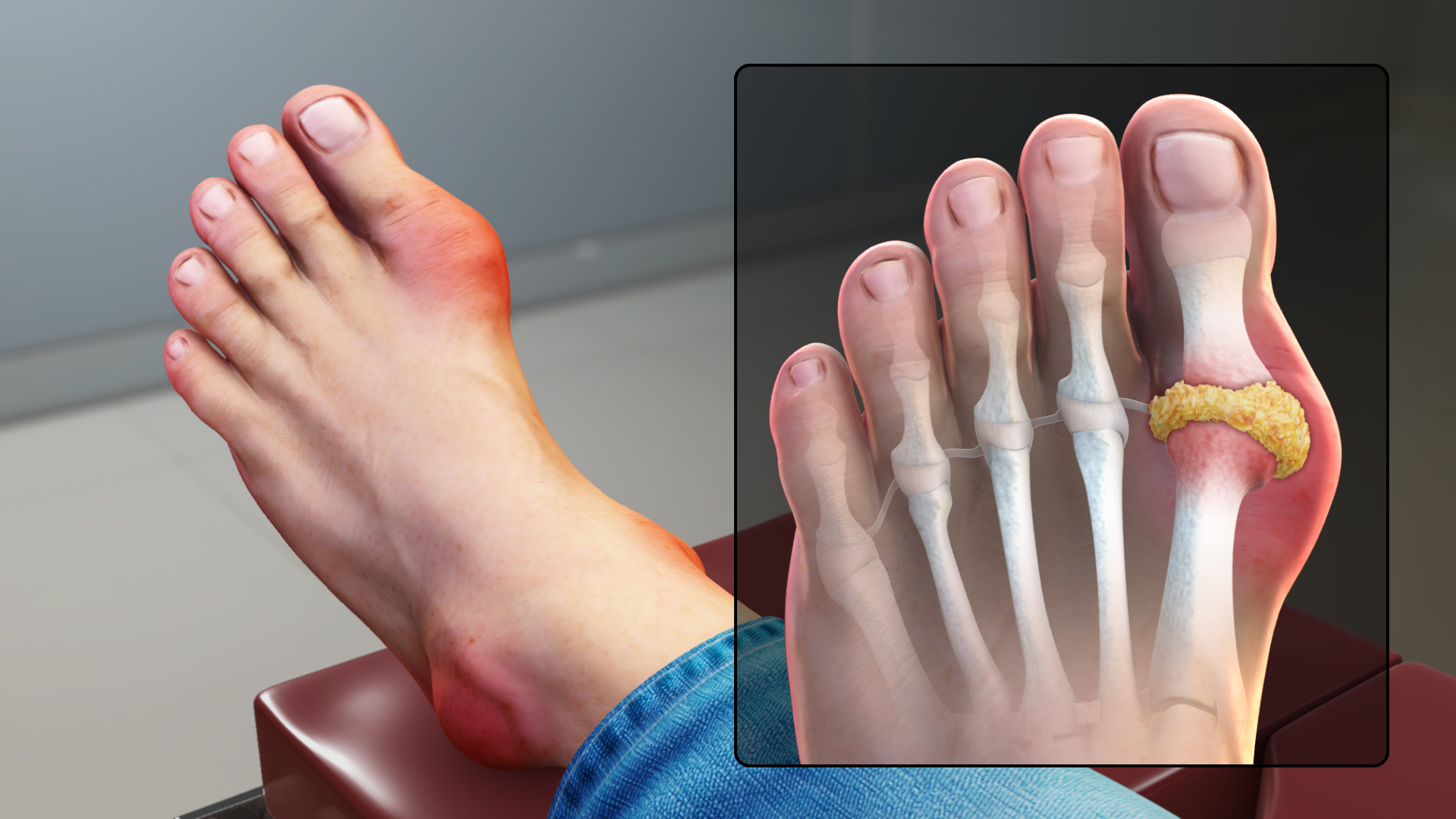
Gout
Often we associate arthritis with older patients who have lived an active lifestyle. Gout, on the other hand, can affect anyone. Gout is a common form of arthritis that is known for its sudden attacks of pain and joint tenderness. Joints that are affected by gout are often hot to the touch, swollen, and very tender. While symptoms are not chronic, it is essential to take preventative measures to manage gout as its side effects can be debilitating and intolerable.
- Stay hydrated. By drinking plenty of fluids and limiting sugary drinks, you can help prevent future gout attacks.
- Maintain a healthy weight as directed by your healthcare provider.
- Limit alcohol consumption. Some types of alcohol are more likely to increase the likelihood of a gout attack.
- Consider adding low-fat dairy products to your diet. These foods are proven to help protect against gout and are excellent sources of protein.
FAQ
What causes gout?
Gout is caused by hyperuricemia. Hyperuricemia is a condition in which the body has an excessive amount of a biochemical called uric acid. We can be overproducers or under execrators of uric acid. Proper diet and exercise help in this condition. Gout was called Podagra over the ages and usually affected the wealthy upper class. As such, it was thought to be a “Rich Man’s Disease” as only the wealthy were able to eat a diet rich enough to produce high levels of uric acid in the body. Now that we generally have plenty of food to go around we are all more at risk for gout as a population. The Diabetic population is also at a higher risk for gout.

Ankle Pain
The foot and ankle are highly specialized structures that absorb the weight of the body and enable us to move. Experts estimate that the force and pressure on your feet when walking can be up to two times your body weight. This pressure can increase with more vigorous movements such as running and jumping. With so much pressure on your feet and ankles, they undergo a lot of wear and tear throughout your life and are highly susceptible to injury and trauma.
The foot and ankle are a complex system of bones, ligaments, muscles, and joints that provide the structure and stability we need to move freely. If any of these components become compromised or weakened due to injury, overuse, degenerative conditions, or sprains, it can significantly impact your foot’s ability to move and function properly.
FAQ
Why am I having ankle pain?
Having a recent injury, like rolling your ankle or falling down, can certainly leave you with ankle pain. But sometimes the reasons behind your pain aren’t as obvious. Common causes of ankle pain include:
- Ankle and foot fractures
- Ankle sprains and strains
- Tendonitis
- Tendon and ligament tears
- Ankle instability
- Arthritis of the foot and ankle
- Wounds
- Trauma injuries
- Sports injuries
What is the treatment for ankle pain?
It depends on your diagnosis. With a soft tissue injury, like a sprained ankle, you may have to go through physical therapy for several weeks to:
- Help your ankle heal properly
- Build strength
- Prevent reinjury
If we determine that you have arthritis, you might need medication or injections to reduce swelling in your joints. But for severe ankle injuries, we may recommend surgery to repair torn ligaments or tendons, or broken bones. Some patients are candidates for total ankle replacement. We specialize in total ankle replacements. Usually, this is the last resort if your ankle still seems unstable after you go through conservative treatment opti0ns.
Can I do anything to relieve ankle pain?
Your ankle just needs time to heal, especially right after an injury. The acronym RICE is helpful for reminding you to:
- Rest your ankle
- Ice it for the first 24-72 hours
- Compress it for the first 24-36 hours
- Elevate it above your heart 2-3 hours per day while it’s swollen
Resting doesn’t mean you have to lie in bed all the time while your ankle is healing — just try to stay off of it as much as possible. Using crutches or a walker can take much of the pressure off your injured ankle while it’s healing.
Will I need to wear a brace?
Possibly. Right after an ankle injury, you should wrap your ankle with a bandage to provide compression. This reduces swelling, but it doesn’t do much to provide support when you put weight on your ankle. Dr. Clark might fit you for a brace, or even a walking cast, if your ankle needs strong support to heal properly.

Shin Splints
Shin splints are painful sensations on the sides of the leg bone caused by muscle or tendon inflammation, usually seen in athletes.
Proper stretching before and after exercising can drastically reduce the occurrence of shin splints. Corrective shoes and/or orthotics can also aid in the prevention of shin splints.
request an appointment
ITB Syndrome
What causes lliotibial Band Syndrome?
The iliotibial band is “ligament on the outside of the thigh extending from the hip to the lateral aspect of the knee. The iliotibial band stabilizes both the hip and the knee during the gait phase.
What is ITBS?
liotibial band syndrome is a condition where an athlete develops pain at the insertion of the ITB at the lateral aspect of the knee or its origin at the hip. Either location can cause considerable pain and disability in an athlete. The disease is often caused by a over-pronation and internal rotation of the hip. Also, this excessive foot pronation causes internal rotation of the knee which can stress the ITB at the knee level. Weakness or substituting muscles about the hip can also cause overuse of the iliotibial band eventually leading to this disease.
Many runners will describe a “snap’ as they extend and flex the knee and/or hip and feel as if the “tendon is tearing”. This is in actuality a compression syndrome as the band of tissue passes over the knee joint (Gerdy’s tubercle) and over the the hip bone. The pain will be diagnosed by taking the knee from an extended position to a partially bent position and back to extended while placing thumb pressure over the lateral aspect of the knee (Gerdy’s tubercle). A similar maneuver can be performed at the hip.
Treatment for ITBS:
- Proper stretching techniques along with lateral hip extension exercises directed through athletic training and physical therapy.
- Nonsteroidal anti-inflammatories as directed by your physician
- Gradual warm-up exercises prior to running workout
- Ice after each workout. (Ice baths are needed on occasion)
- Cross training through cycling and swimming
- Biomechanical examination to obtain a proper diagnosis
- Functional orthotics (these may be designed to reduce pronation in most instances, however, for those unique individuals with minimal pronation and a very high arch we may need to take a different tact to increase flexibility and hip rotation)
- Specific shoes types specific to your mechanics
Tip: Dr Francis Clark researched ITB syndrome while in medical school and presented a paper on the disease and it’s treatments. He provided an early study that recognized the disease in those with cavus feet who had minimal pronation. As such, he proposed that the disease of ITBS affects those at both extreme ends of the spectrum of hip and knee rotation. As such, he is always up for a challenging ITB case and loves to get his runners back on the road.
